Myths about COVID-19 busted: Masks, indoor transmission, cold weather, and more

CHICAGO -- University of Chicago Medicine Executive Medical Director for Infection Prevention and Control Dr. Emily Landon took time to bust some of the most prevalent myths about COVID-19 and the pandemic, as coronavirus cases continue to rise across the nation.
Inconsistent recommendations or data are not evidence of conspiracy
Since the start of the pandemic, information about COVID-19, its effects, symptoms, modes of transmission and prevention has changed consistently, leading some to question whether the information can be trusted.
It can, Landon said, and should. There is no one metric that works in every situation, and sometimes doctors and public health experts use different metrics in different contexts to make decisions.
New data comes in every day as science continues to learn, Landon said, which can lead to disagreements, but disagreements are a normal part of the scientific process.
"We change our guidance because we learn something new," she explained. "Changing advice should make you feel good about our making progress. Disagreement is a normal part of every process, and there is no right way to handle a new pandemic. But we're all in the same boat and we should try to row in the same direction as much as possible."
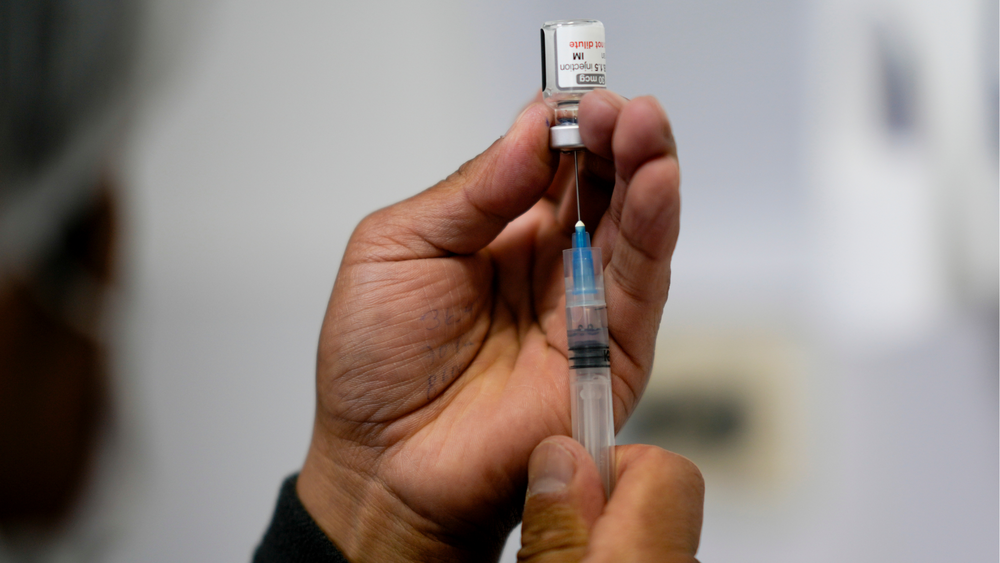
Don't be skeptical of masks: they work
Landon fully admitted some of the guidance on masks may have been confusing to the public because doctors and scientists simply did not know in March how important they would be for curbing transmission.
"Every single study now shows that masks reduce risk," Landon said. "Common sense says that masks reduce risk. Healthcare workers would all get COVID when they were caring for patients if masks didn't prevent infection, and studies of healthcare worker antibodies show that they have had COVID only slightly more than the regular population, despite having very close contact with patients who have COVID."
No mask is perfect, but Landon said there is a growing body of evidence that if you get COVID-19 while wearing a mask, you may not get as sick. That means that mask wearing also appears to be related to the lower levels of mortality as the pandemic has progressed, according to Landon.
She also emphasized the importance of mask mandates, pointing to a study in Kansas that showed that counties that had mask mandates had both overall lower rates of COVID-19 and lower rates of mortality than counties that did not have mask mandates.
According to Landon, wearing a mask may reduce the severity of COVID-19 illness and consistent usage of masks is crucial to preventing transmission.
She also emphasized that face masks are absolutely safe, and pointed out that all kinds of people - from health care workers and doctors to construction workers and artists - have been wearing masks for long periods of time without any complications and negative effects.
Her main point: Masks are safe and you must wear one in order to control the spread of COVID-19.
Fall and winter will make COVID-19 transmission worse
Doctors and public health experts have been warning that COVID-19 would come roaring back in fall and winter, for several reasons that have to do with the season itself, including temperature and air.
The moisture in humid, warm air keeps COVID-19 from spreading, Landon explained. The virus gets caught up in the droplets of moisture in the air, which weigh more and fall faster, preventing the virus from traveling as far as it can.
Cold air, by contrast, is drier and HVAC systems in homes and businesses are bad at creating or maintaining humidity. We know this, Landon said, through the things we typically do during winter like use more lotion to combat dry skin, or purchase humidifiers to help with the air in our homes.
The drier air lets the COVID-19 virus hang longer, fall later, and travel farther, Landon said. That means it can be transmitted more easily through airborne transmission.
Landon said the cold weather also makes us stay inside, in our energy-efficient homes that so effectively keep in both heat and virus. Because of that we are most at risk from what Landon called the "Three C's: Unmasked contact in a closed space that's crowded.
Landon said studies have found that indoor ventilation in most buildings is not enough to prevent COVID-19 transmission without masks. That is one of the reasons bars and restaurants carry a higher risk of transmission; it's not possible to eat and drink while wearing a face covering.
As a result, it is crucial to limit indoor gatherings, from break room lunches and small book clubs to larger gatherings like eating out or large family holiday celebrations.
"I know you miss your family and your friends, and some days you probably don't even care if you get COVID," Landon said. "But you do care. We all care."